The health report the government won't publish

The health services knew about the appalling conditions at Leas Cross from October 2004, but took no real action until Prime Time exposed the scandal. By Sara Burke
Patients in Leas Cross lived significantly shorter lives than those in other nursing homes. In particular, vulnerable patients who had been transferred from St Ita's psychiatric hospital in Portrane lived for an even shorter time.
Leas Cross residents were neglected and abused. There were far too few nursing and medical staff, the rate of bedsores and use of restraints was way above international standards, overall standards of care were very poor – Des O'Neill describes them as "abusive".
Even more significant is that the Eastern Regional Health Authority and (since January 2005) the Health Services Executive had been made aware of these abuses by relatives of patients and senior medical staff, most notably those in St Ita's Hospital, but nothing was done.
From October 2003, consultants in St Ita's hospital made their serious concerns clear to health-service management in a series of letters to no avail.
Also, no one has been held to account for the poor quality of care that was allowed to prevail in Leas Cross.
Des O'Neill says in his report there is no reason to believe that abuse like this was not happening in "to a greater or lesser extent" in many long-term care facilities for older people.
While progress is being made on inspections of nursing homes, legislation has yet to go through the Dáil to establish a Social Services Inspectorate for old people's homes.
The following is an edited version of a draft report – 'A Review of the Deaths at leas Cross Nursing Home 2002-2005' – written by Desmond O'Neill, consultant geriatrician in Tallaght Hospital, in January 2006.
Leas Cross Nursing Home in 2005
Leas Cross was a large nursing home by Irish standards, registered for 111 beds in 2004 (the median number of beds in nursing homes in the Eastern Regional Health Authority was 45). Leas Cross had a very complex case mix where the majority of patients had a high dependency level.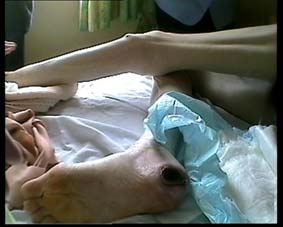
A total of 105 deaths were detected between 2002 and 2004. The register [of patients] was poorly maintained, with no stated destination (where they went to after leaving) or death declaration for 439 out of a total of 690 (64per cent). Although some of these could be identified as repeated short stays (presumably to provide respite for those caring for the patients at home) and others were individual short stays, in at least three cases, the death of the patient was not mentioned on the register.
In general, the column [in the register] for indicating the (statutory) obligation to report death to the health board was left vacant. There are discrepancies between the number of admissions in the register and the returns made to the health board for the annual report on long-term care by the Department of Health in three of the four years when returns were made: no returns were made for three of the seven years involved.
PATTERNS OF DEATH
It is a source of concern that no government or health agency knows the death rates in Irish nursing homes.
I could only detect one [relevant] published Irish study... [this was a study of the time spent by patients in nursing homes following transfer from St James Hospital].
The median duration of survival, between the years 1997 and 2000, varied from 17 to 44 months... In Leas Cross, the median time to death of those who died was 221.5 days (7.3 months) from all hospitals, but only 77 days (2.5 months) for the St Ita's patients (ie patients transferred from St Ita's psychiatric hospital in Portrane). This was a particular cause of concern and mirrors concern expressed in strong terms by the consultant psychiatrists in St Ita's Hospital to [named health services managers].
There is an almost complete absence of systematic monitoring of deaths in Irish nursing homes...
Deaths reported to the Health Board/ Health Services Executive (HSE)
There is a statutory obligation to report deaths in nursing homes to the Health Board/HSE. Only 31 of 60 notifiable deaths were notified to the health board, of which 16 were received on foot of a request from the Senior Area Medical Officer...
Death notified to the coroner
Since July 2004 there has been a ruling by the coroners that deaths of residents in nursing homes [must] be referred to the coroner's office. Of those who died in Leas Cross in July 2004, eight were referred to the coroner and eight [others] were not, a compliance of 50 per cent. Of those who died in Beaumont [Hospital, having been transferred from Leas Cross] from July 2004, six were referred to the coroner and 10 [others] were not, a compliance of 38 per cent...
The coroner's reporting system is an important mechanism for detecting concerns over any issues that might arise from deaths of nursing home residents... Where the coroner decides to investigate more fully, the investigation is thorough and in the case of one death in Leas Cross provided an insight into poor quality of care, which resulted in a verdict of "death by misadventure". The transcript and the verdict of the case of Dorothy Black [a patient at Leas Cross whose treatment and death was documented in the Primetime programme] represented a telling indictment of the standards of care, which are mirrored in the absence of adequate and satisfactory documentation of appropriate nursing care.
REVIEW OF [LEAS CROSS] NURSING HOME CASE NOTES
In general, the filing and maintenance of the case notes was deficient in many respects. Not only were important basic data missing, but the structure of the notes was counterproductive to care planning for this patient [Dorothy Black]...
Weight
Only 11 of 107 patients (10 per cent) have weight recorded on admission. This is important... because malnutrition is common and a serious problem in nursing homes and good nursing care requires a baseline weight... It [weight recording] is a marker of the standards of nursing care and it is required by nursing home regulations.
Skin condition
Only 15 out of the 107 (14 per cent) had skin conditions recorded on admission... This is again important... Given the high prevalence of disability in Leas Cross, many would be at risk of developing pressure sores... Failure to record skin condition is also a mark of the standard of nursing care...
Pressure-sore prevention and care
Pressure-sore prevention and care is a key indicator of quality care for vulnerable people in residential care... [It] has been selected as one of the eight core areas of quality assurance by the UK Department of Health... In some jurisdictions severe lapses of pressure-sore care leading to death have successfully been pursued by government agencies as homicide, most notably in Hawaii.
The care in Leas Cross raised grave concern in the case notes reviewed. Pressure sores were documented at one stage or another in 33 of 100 available notes... The inadequate documentation and lack of clear care routines for pressure sores are notable in one of the cases which entered the public domain, that of Dorothy Black: in her case the coroner entered a verdict of "death by medical misadventure"...
Restraints
An alarming number of residents were being noted as being nursed in Buxton chairs [restraining chairs]... Nursing homes with a high use of restraints are associated with low performance on a number of quality care indices.
Medical cover
Medical cover was almost exclusively provided by a single medical officer at any one time... The Nursing Home Inspection Team [set up by the Northern Area Health Board in October 2004 to inspect nursing homes]... [requested] clarification from the [Leas Cross] nursing-home proprietor as to whether a single GP could provide a level of input adequate to the needs of – potentially – 111 patients... The case of Dorothy Black clearly raises serious concerns [about medical care]... In pressure-sore care and only in a very small number of the 33 cases [where the sores were documented] was there a medical note observing the pressure sores.
In two instances the nursing notes note difficulty in contacting a doctor, in one case extending for three days... Concerns arise out of deferring assessment to the next day for one patient [who had] very high sodium and urea and who was subsequently transferred to hospital and died shortly thereafter. There was no evidence of a policy of [the management of] dysphasia [difficulty with swallowing], although a significant minority of those who died in Beaumont [Hospital] were detected of having this significant disorder...
Nursing staff
The staffing at Leas Cross was clearly deficient in terms of expertise, nursing numbers and nursing infrastructures. This is perhaps the single most grievous area of concern of practice within the nursing home, and many other problems arise from this fact. Quality nursing time is... associated with better care and outcomes and there is no evidence that this was appreciated at any level in Leas Cross...
Care-assistant staffing
Care assistants play an important role in the complex and sophisticated care of older people... care assistants also require formal training... There was no evidence of any vocational training of the care assistants staff in Leas Cross.
Therapist staffing
Among the striking findings... at Leas Cross was the virtual complete absence of documentation of formal input by physiotherapists and occupational therapists. It is clear that this frail group of older people will not only require physiotherapy but also occupational therapy, clinical nutrition and speech and language therapy...
Specialist medical input
The provision of services by old-age psychiatrists and geriatricians was an important part of both support to the older people in the nursing home but also played an important role in bringing cases of poor quality care to the attention of the health services and the coroner. Both services have documented the fact that their resources were very stretched by trying to support the large group of frail people in nursing homes...
OFFICIAL OVERSIGHT OF LEAS CROSS
Nursing home inspection team
Prior to October 2004 there was no designated team assigned specifically to the inspection of private nursing homes in the Northern Area Health Board. Inspections were conducted at an area level by [individuals from a specified pool of health-board medical personnel].
Following a change in October 2004, a designated team was set up consisting of [three senior health-board appointees]. The sequence of [their recorded] visits portrayed a consistent pattern of deficits in care [in Leas Cross]. Prior to the new format of inspection, the [inspection] reports for Leas Cross [had been] relatively brief with significant focus on physical surroundings.
The first break with this was an individual report (22 January 2004) following the death of Dorothy Black, which outlined a complete lack of formal assessment, procedures or protocols for pressure sores, as well as scantily informed documentation with no evidence of appropriate care, inadequate staffing and skill mix. These issues would be a recurrent refrain over the next 18 months, and the report concludes with the perception that Leas Cross was working with the Northern Area Health Board to correct these deficits, again a recurrent refrain...
This report of 13 July 2004 outlined severe deficiencies in staffing, skill mix, senior nursing structure, health and safety... medical regulations, nursing care standards and access to the doctors...
A report of 10 March 2005 details concerns over skill mix and staffing...
The inspection of 7-8 April 2005 highlights the deficits in staffing; communication and continuity of care; adequacy of records provided... adequacy of drug-administration records; notification of deaths to the health board; and requested clarification of the adequacy of medical care provided.
The patterns of reporting in subsequent inspections, with one exception, show ongoing concerns over the standard of care... A letter of 23 June 2005 detailed the results of a further inspection, including breaches of good nursing practice, professional guidelines and the Misuse of Drugs and Regulations Act...
A further letter describes breaches of the nursing home regulations. At this stage the nursing home inspection team declared that on the basis of their findings, the current staffing and skill mix did not support good safe practice in the delivery of care, given the number and dependency level of patients. What might be termed as a final inspection report was written by [named personnel] following the putting in place of a team from the HSE [after the Primetime documentary, which aired in May 2005] to try to run the nursing home. This was a devastating amplification and clarification of the many concerns of the nursing inspection team dating back to the April visit. [The HSE withdrew all patients from Leas Cross in July and the nursing home closed in August 2005.]
[Two other reviews were carried out on Leas Cross. The following refers to one of these.]
As a result of a different inspection process by the ERHA [Eastern Regional Health Authority]... the assessors were concerned with what they found... on the second visit of 15 March 2005, it failed in the areas of quality of premises, acceptability to users and referrals, versatility... This was followed by a letter from [a named health service manager] (4 April 2005) requesting clarification from [a named inspector] as to the standard of care. This again should have been taken as a warning signal of the gravest import.
In his reply to the [named health service manager] on 13 April 2005, presumably drawing on his visit of the 7-8 April, [the named inspector] expresses concern [about] the care needs. His concerns included (a) adequacy of medical care... and... (b) skill mix... [It] concluded that there was no immediate danger to current residents. He also notes that the HSE (Northern Area) did not have data on death and death rates in the 30 nursing homes in the area.
COMMUNICATIONS TO THE NURSING-HOME INSPECTION
TEAM
Perhaps the most worrying aspect of the failure of the nursing-home inspection-team process (including senior management) was the failure to address a very serious concern raised by... relatives [of residents] about deficiency in care and oral and written communications from mental-health professionals around the time of transfer of patients from St Ita's Hospital
My overall impression is that the concerns raised in the complaints to the HSE were very serious in nature and do not seem to have triggered an appropriate response. In particular, there seems to be a marked failure to recognise the gravity of negligence in pressure-sore care. In the case of Dorothy Black, [a senior health-board person identified in the report] who was enjoined to review the medical care commented that "the general care of the lady did seem adequate with the exception of pressure sores". Given that the pressure sores were, in the large part, the cause of her death, this does not seem to represent an appropriate response but is also a reflection that the team did not use special medical assessment... A letter from a senior HSE manager to the family does not seem to recognise that the care in the case represented a catastrophic lapse in service provision which was unlikely to represent an isolated incident... Most of the other complaints from family members are consistent with poor care reflected in the notes and in the nursing-home inspection report and should have triggered a more prompt and muscular response.
SEQUENCE OF COMMUNICATIONS FROM MENTAL-HEALTH
SERVICES TO THE ELDERLY RE LEAS CROSS
At the end of October 2003, concerns [were] raised by Dr Mary Cosgrove [consultant psychogeriatrician at St Ita's Hospital] over the need for follow-up of the patients' transfer from St Ita's Hospital to nursing homes... A letter [was sent] within two weeks to [named health service manager]... Drs Cosgrove and Piggot [another consultant in St Ita's] particularly [brought] attention to the fact that three of the initial group of 14 patients discharged to Leas Cross nursing home had been referred to Beaumont Hospital and all had been quite seriously ill. They noted that nursing care appeared to have been the issue in all of these and the last two patients had arrived with bronchial pneumonia... and one with dehydration...
These concerns were amplified in the letter to [named health service manager] on 9 January 2004. They pointed out that seven deaths had occurred since the transfer in September, three of which occurred over the Christmas period. Dr Cosgrove pointed out that Dr Kieron Donegan, consultant geriatrician in Beaumont Hospital, spoke to the coroner [about] these deaths as there was a question of decubitus ulcers [which result from pressure sores] and where they were acquired. Dr Cosgrove was clearly sufficiently concerned to [subsequently] contact the coroner's office to let them know of the death of a second patient. This letter was widely circulated...
In a [different] letter of 27 April 2004 to [a named health service manager circulated to two other unnamed but identifiable health service managers], Dr Cosgrove points out again that she had significant concerns over the discharge initiative and particularly the deaths occurring in one nursing home – Leas Cross. She also expressed concerns about the nursing-home regulations in terms of inspection process and powers of inspectors, staff levels and skill mix of staff, in particular the numbers of qualified staff and staff training...
In a letter on 30 April 2004... Dr Cosgrove... clearly states concerns from both herself and Dr Donegan of care in private nursing homes. This letter neatly summarised the concerns that, in the absence of adequate public extended care facilities, that the private sectors, as currently configured in nursing homes, cannot deal adequately with end-stage dementia or patients with behavioural disturbance and that financial or other possible trends may be limiting the Health Board from contracting more expensive, but what are perceived to be better, care...
Dr Cosgrove highlights that the main problem encountered on review visits was the lack of qualified staff and auxiliary staff and basic care to meet the patients' needs... Of some concern were her findings from interviewing patients who were residents. A percentage of patients complained of inappropriate use of incontinence pads, and ambulant patients' shoes were missing for two days and relatives who were visiting at the time expressed concerns to Dr Cosgrove. Four of the former St Ita's patients were sitting in wheelchairs and others in Buxton chairs. General personal hygiene was poor. Clothes were grubby in appearance and a few patients had a strong odour of incontinence... The staffing appeared inadequate...
These concerns were also discussed with [a named health service manager].
A further matter of significant concern raised by the consultant psychiatrist was that the group with dementia as a primary diagnosis had a higher mortality rate in Leas Cross. The admissions that were transferred to hospital were characterised by dehydration, aspiration pneumonia and skincare problems raising concerns over adequacy of care...
In a further letter of 7 October 2004, Dr Cosgrove and Dr Piggot point out... the difficulties with respect to the care of patients raised in relation to numbers of qualified nursing staff – they point out that in some cases the nursing ratios are very low, just one nurse and a number of care attendants looking after perhaps 40 or 50 patients. This can only be noted as a very serious indicator of concern on behalf of the consultants of old-age psychiatry about the adequacy of care in nursing homes.
Drs Cosgrove and Piggot clearly point out the problems encountered with previous discharge initiatives to nursing homes in a further letter of 2 April 2005 to [named health service manager].
Following this, a letter of 6 April 2005 from [a named person] noted the request of... [St Ita's] to cancel six beds in Leas Cross Nursing Home and move them to other nursing homes. [In a subsequent letter]... Dr Cosgrove... noted that she had repeatedly transmitted concerns by correspondence to various levels of the [Northern Area Health Board]/HSE (NA) management regarding issues arising at Leas Cross Nursing Home and, in particular, the lack of qualified staff on the ground and also commenting that a health board paying as low a price as possible for beds may not be giving nursing homes a chance to provide top-quality service.
Questions put to the HSE by Village about Leas Cross
We put a series of questions to the Health Services Executive (HSE) and the Department of Health and Children on the Leas Cross report. The following are the questions and the answers we received (unless stated all responses are from the HSE):
When will the Leas Cross report be published officially?
It can't be published in its present form but we are anxious to publish it soon and hope to do so in the next two to three weeks. We are looking at three or four options which may get around legal options in publishing the report in its present form.
Has any one individual in the health services been held accountable for the poor standards and care in Leas Cross?
There was a systems failure which has been acted upon, for example the complete reform of nursing home inspection. [The press officer declined to comment on whether anyone will be held to account.]
What action has been taken since the screening of the Primetime programme in May 2005 to ensure quality care in private nursing homes?
• The Working Group on Nursing Home Inspections and Registrations produced a report in July of this year which now underpins our inspections process and which places much greater emphasis on patient welfare. This new National Private Nursing Homes Inspection Process has established a national, uniform, consistent inspection process. Inspection teams are now carrying out inspections across the country using a consistent framework.
• As part of this process, there has been significant engagement with the Private Nursing Homes Sector and the Nursing Homes Inspection Teams.
• A training programme for inspection-team members is being developed.
• Resources have been identified for dedicated nursing home inspection teams.
• We are currently hiring 32 Elder Abuse Officers and the recruitment process is at an advanced stage. These will be in place by the end of the year.
• The HSE last September began publication of inspection reports on the HSE website. These reports are based on inspections carried out since July and reflect the new inspection process that was introduced at that time.
When will the Social Services Inspectorate have responsibility for inspecting nursing homes?
This year, the Minister for Health and Children carried out a public-consultation process on the draft scheme and heads of a bill to establish the Office of the Chief Inspector of Social Services within the Health Services Information Authority, with specific statutory functions. Following on from that process, the intention is to bring a bill to government for approval this session.
The remit of the Social Services Inspectorate is being widened to include residential care for people with disabilities and older people. The Office of the Chief Inspector of Social Services is being established within HIQA [Health Information and Quality Authority] and will be given specific statutory functions. The functions of the Chief Inspector of Social Services will be to establish registers for residential centres for people with disabilities, children in need of care and protection and older people, including private nursing homes. The Chief Inspector will have powers to inspect centres, register centres, attach condition to registration and cancel a registration. The Chief Inspector will also inspect the HSE's performance of its functions in respect of foster care services, boarding out of older people and inspections of pre-schools. (Department of Health and Children).
